
Most IVF clinics don’t have a patient problem.They have a visibility problem.
On the surface, everything appears to be working. Your team is busy, consultations are happening, cycles are being managed, and patients are moving through the system. But when you step back and look at outcomes, something feels off.
Some patients never return after consultation.Some cycles don’t convert as expected.Growth feels slower than the effort being invested.These aren’t random issues. They’re signals.And more often than not, they point to one underlying challenge: IVF clinic data gaps.
These gaps don’t show up as clear failures. They exist quietly between processes, between teams, and between systems. But over time, they shape your clinic’s efficiency, patient experience, and revenue in ways that are hard to ignore.
What Are IVF Clinic Data Gaps (And Why They Matter More Than You Think)
In an IVF clinic, data is generated constantly.Every patient interaction, every test result, every cycle update adds to a growing pool of information. But the challenge isn’t the absence of data. It’s the lack of continuity in how that data is captured, connected, and used.
A patient may complete a consultation, but the outcome of that interaction isn’t systematically tracked.A clinician may make an observation during a cycle, but that insight doesn’t get translated into broader learning.A front desk team may follow up with a patient, but that communication isn’t visible to the clinical team.
Over time, these small disconnects accumulate.What you’re left with is a system where:
- data exists, but context is missing
- insights are possible, but not accessible in time
- decisions are made, but not always informed by the full picture
This is what defines a data gap in the IVF context.And the impact isn’t theoretical. It shows up in very real ways: missed conversions, delayed interventions, inconsistent outcomes, and ultimately, revenue that never materializes.
How IVF Clinic Data Gaps Impact Patient Conversion and Revenue
Every IVF clinic invests heavily in attracting patients and delivering high-quality care. But between those two points lies a complex journey, one that depends heavily on timing, communication, and coordination.
When data gaps exist, that journey becomes fragmented.A patient who leaves a consultation with unanswered questions may not return, not because they aren’t interested, but because no structured follow-up was triggered.
A delay in identifying a pattern during stimulation may reduce the chance to adjust treatment in time.A lack of clarity on conversion rates may lead to missed opportunities for improving patient experience.What makes this challenging is that these issues don’t always appear in reports. They don’t show up as clear losses. Instead, they appear as “missed possibilities.”And over time, those missed possibilities compound.
Clinics often describe this as a feeling that they could be doing better, without being able to pinpoint exactly where the gap lies. That intuition is usually correct. It’s just that the underlying data isn’t visible enough to confirm it.
The IVF Journey: Where Visibility Begins to Break
The IVF journey is often described as a linear process, but in reality, it is far more dynamic.Patients move between stages, ask questions, pause, reconsider, and require reassurance. Each of these moments generates data, but not all of it is captured or connected.
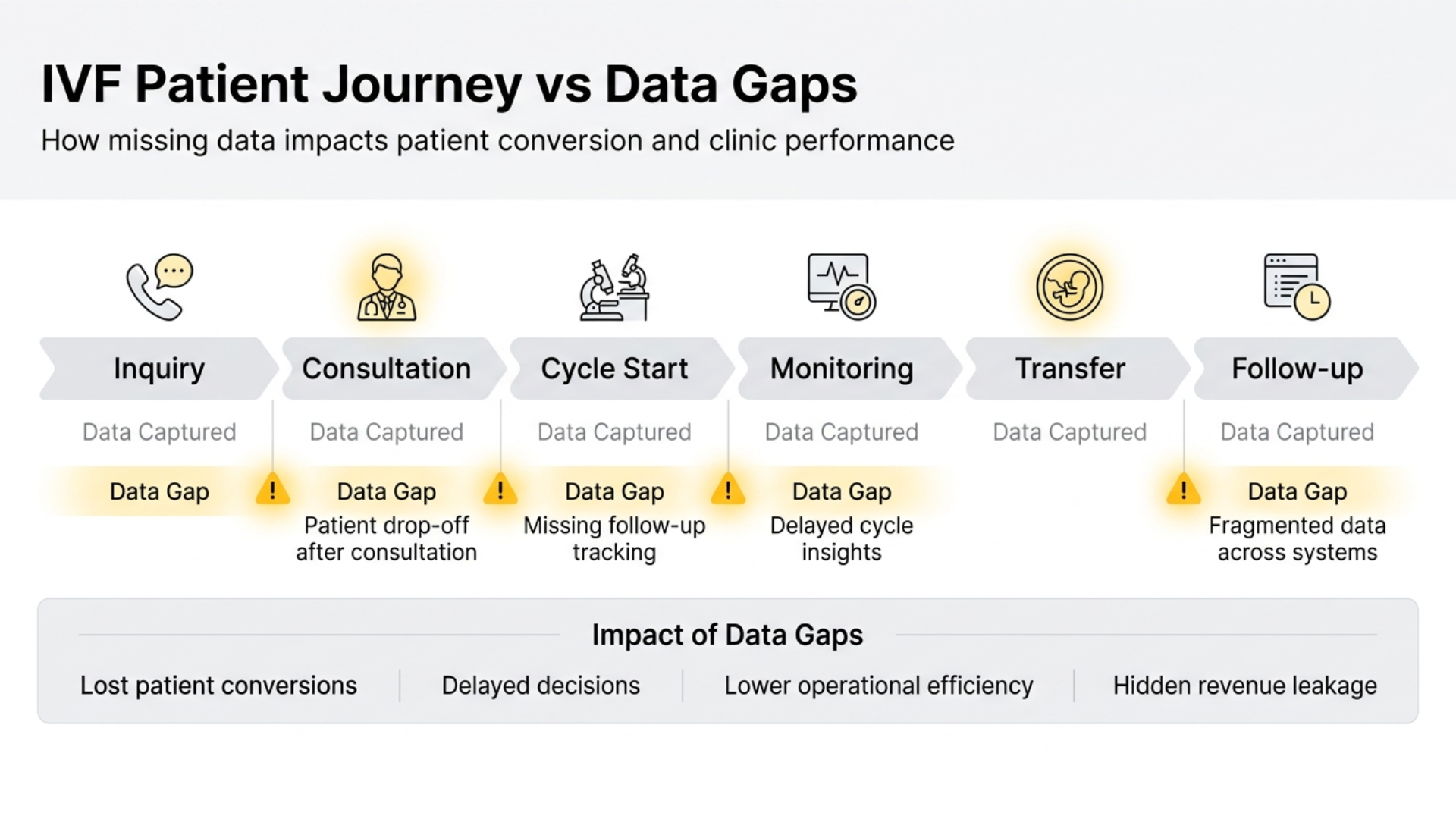
When you map the journey visually, from inquiry to post-treatment follow-up, something becomes clear.The points where patients are most uncertain are often the same points where data visibility is weakest.Without a connected view of this journey, it becomes difficult to understand not just what is happening, but why it is happening.
7 IVF Clinic Data Gaps That Quietly Drain Revenue
1. Patient Drop-Off After Consultation
This is one of the most significant and least understood gaps in IVF clinics.
A patient expresses interest, schedules a consultation, engages with the clinician, and then does not proceed. In many cases, this is treated as an isolated event. But when it happens repeatedly, it points to a deeper issue.
Without structured tracking, there is no clear answer to why patients are not converting. Was the information overwhelming? Was pricing unclear? Did they seek a second opinion?
More importantly, there is no system in place to re-engage them at the right time.
This gap sits at the intersection of patient experience and revenue. Every missed conversion here represents not just a lost patient, but a lost opportunity that could have been recovered with better visibility.
2. Fragmented IVF Patient Data Across Systems
In many clinics, different teams rely on different tools. The front desk manages appointments, the lab tracks embryology data, clinicians maintain their own notes, and financial teams operate separately.
Each system functions well in isolation. But IVF is not an isolated process.When these systems are not connected, the patient journey becomes fragmented. A clinician may not have full visibility into patient interactions. A lab may not be aware of communication gaps. A manager may not see the complete performance picture.
The result is a clinic that is working hard, but not always working in sync.Over time, this fragmentation leads to inefficiencies that are difficult to diagnose because no single system reflects the full reality. If you want to read more about it, refer to – https://meddilink.com/blog/how-to-manage-fragmented-data-in-ivf-clinics/
3. Lack of Real-Time IVF Cycle Monitoring
IVF is a time-sensitive process where small adjustments can make a meaningful difference.But when insights are delayed, those adjustments become reactive rather than proactive.In clinics where reporting relies on manual compilation, data often arrives after the fact. By the time patterns are identified, the opportunity to act has already passed.
This doesn’t always result in immediate visible consequences. But over multiple cycles, it affects consistency and outcomes.
Real-time visibility changes this dynamic. It allows clinicians to act with confidence, not hindsight. To know more, click here
4. Untracked Patient Communication and Engagement
For patients, IVF is not just a medical process. It is an emotional journey filled with uncertainty.
They rely on timely communication, clear explanations, and consistent support. When communication is not systematically tracked, it becomes dependent on individual effort rather than structured processes.
This creates variability.Some patients receive timely follow-ups, while others fall through the cracks. Some concerns are addressed quickly, while others remain unresolved.From the clinic’s perspective, this may seem like a minor operational issue. But from the patient’s perspective, it directly impacts trust.
And when trust wavers, decisions are delayed or abandoned altogether.
5. Incomplete IVF Clinic KPI Tracking
Most clinics track outcomes such as success rates. But fewer track the journey that leads to those outcomes.Metrics like consultation-to-cycle conversion, time delays between stages, and drop-offs at specific points provide valuable insight into how the clinic is functioning.
Without these metrics, performance remains difficult to interpret.A clinic may see stable success rates but declining conversions, or increasing inquiries but stagnant cycle numbers. Without detailed tracking, these patterns remain disconnected.
This is where data moves from being informative to being actionable.
6. No Clear Link Between Clinical Data and Revenue
Clinical excellence and financial performance are often viewed separately, but in reality, they are closely connected.Different treatment pathways, patient segments, and operational efficiencies all influence revenue outcomes.
When clinical data is not linked to financial metrics, it becomes difficult to understand which areas are driving growth and which are creating inefficiencies.This limits the ability to make strategic decisions.Instead of optimizing based on insight, clinics continue operating based on assumptions.
7. No Predictive Insights for Better Decision-Making
Most clinics rely on historical data.They review past cycles, analyze outcomes, and make adjustments for the future. While this is valuable, it is inherently reactive.
Predictive insights introduce a different approach.By identifying patterns early, clinics can anticipate patient behavior, optimize treatment plans, and allocate resources more effectively.This is where the shift toward advanced analytics and AI begins to create a meaningful difference.
Closing the Gaps: What Changes When Systems Come Together
At some point, the pattern becomes clear.These gaps are not isolated issues. They are symptoms of a broader limitation, one where data exists but is not fully connected.Trying to solve this manually often leads to more complexity. More spreadsheets, more follow-ups, more effort. But the underlying issue remains.
This is where unified systems begin to change the equation.Solutions like MedART EMR are built to bring the entire IVF workflow into a single, connected environment.
Instead of managing separate systems, clinics gain a unified view of:
- the complete patient journey
- real-time cycle progress
- communication history
- operational and financial insights
What this enables is not just efficiency, but clarity.Clinics can identify exactly where patients are dropping off, where delays are occurring, and where outcomes can be improved.And once that visibility is in place, decision-making becomes more precise, more timely, and more effective.
If you find it difficult to answer simple questions like how many patients move from consultation to cycle initiation, it may be a sign that the issue is not effort, but visibility.
A Practical Way to Start
You don’t need to transform everything overnight.But you do need to start by understanding where your visibility is limited.Even a focused review of your patient journey can reveal:
- stages where tracking is inconsistent
- gaps in communication
- delays that are currently hidden
For a deeper perspective on how fragmented data impacts IVF clinics, this is worth exploring:
Conclusion: IVF Clinic Data Gaps Are Invisible, Until You Address Them
IVF clinic data gaps rarely present themselves clearly.They appear as patterns that don’t fully make sense. As growth that feels inconsistent. As outcomes that don’t always reflect the effort behind them.
But once you begin to identify them, the shift is significant.You move from uncertainty to clarity.From reactive decisions to informed ones.
From fragmented processes to connected systems.And for many clinics, that shift begins with adopting unified platforms like MedART EMR, where data is no longer scattered but structured, visible, and actionable.
If there is a sense that your clinic could operate more efficiently or convert better with clearer insights, that instinct is worth exploring.Because often, the difference between where a clinic is today and where it could be lies in something surprisingly simple.
Not more effort.But better visibility.
Topics



