Picture the consultation room. A couple sits across from a fertility specialist; nervous, hopeful, rehearsing questions they’ve carried for months. At some point, the doctor’s eyes drift from theirs to the screen. The keyboard starts clicking. The room shifts, imperceptibly, unmistakably, from a medical encounter to an administrative exercise.
This is the problem an AI medical scribe for IVF is designed to solve. Not documentation in general, but the specific, complex, high-volume documentation burden that fertility medicine places on specialists every single day. The question is whether the solution you’re considering was built for that burden, or whether it’s a general-purpose tool being retrofitted.
That distinction defines everything that follows. This blog covers what the technology is, the problem it solves, the data behind the outcomes, and what separates a truly IVF-native solution from everything else on the market.
What Is an AI Medical Scribe for IVF Clinics and How Does It Actually Work?
An AI medical scribe for IVF is an ambient listening tool that sits quietly in the background of a live consultation. It securely captures the doctor–patient conversation, transcribes it in real time using medical-grade speech recognition, the same voice-to-EMR software now used by leading health systems globally, and applies natural language processing to extract clinically relevant data, automatically populating structured fields in the clinic’s EMR. No typing. No dictating. No interrupting the flow of care.
When the consultation ends, a fully structured draft clinical note is already waiting in the EMR. The doctor reviews it, edits if needed, and approves. That review typically takes under 60 seconds.
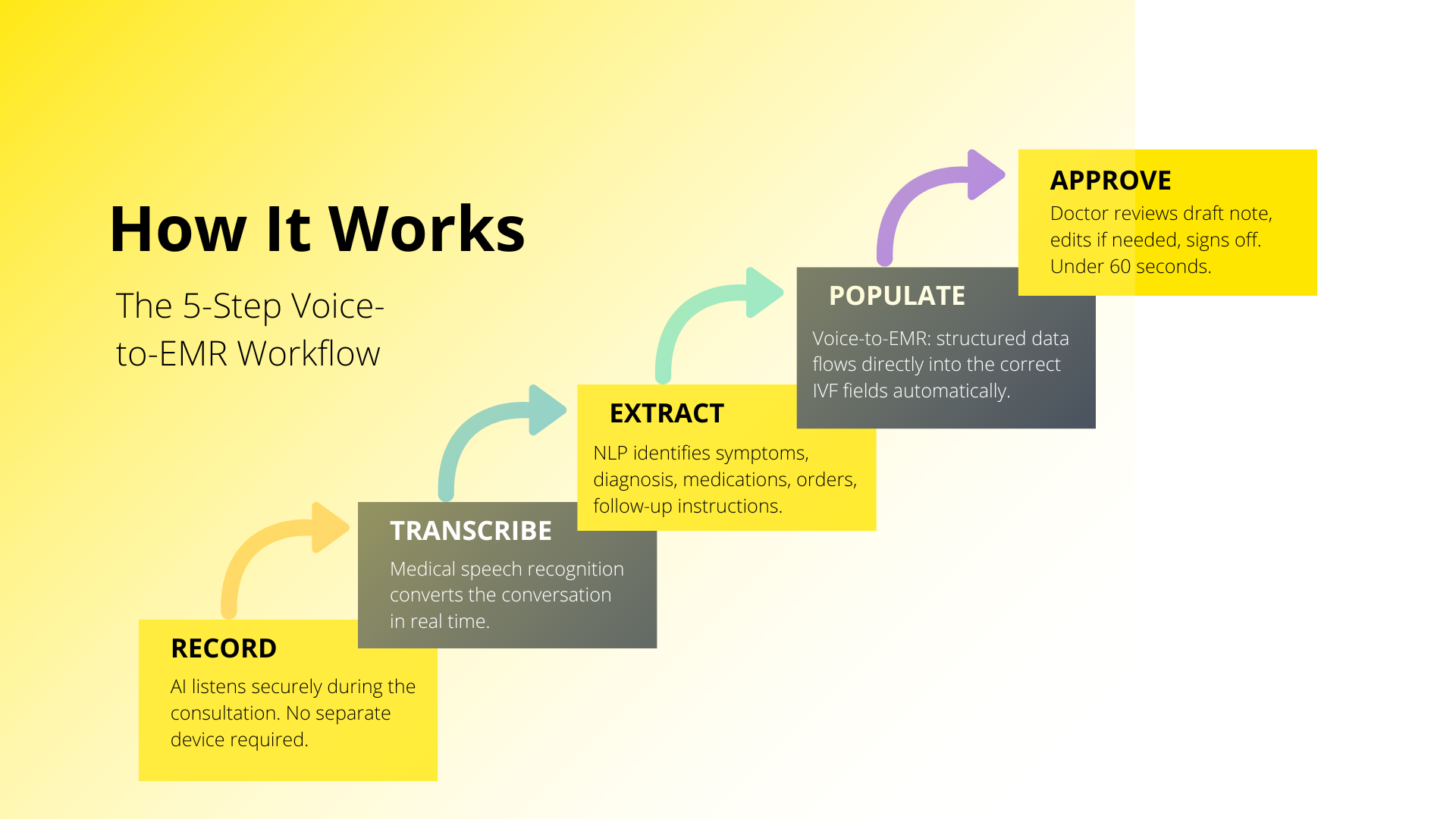
What It Captures in an IVF Consultation
Unlike general medical transcription software, an AI medical scribe for IVF is configured to capture the full depth of a fertility consultation, not just symptoms and diagnosis, but the entire clinical picture a fertility team depends on:
- Chief complaints, presenting history, and previous cycle outcomes
- Ovarian stimulation protocol details, antral follicle counts, and medication dosages
- Oocyte retrieval, fertilisation rates, and embryo development observations
- Diagnosis, clinical rationale, and prescription details
- Lab and imaging orders, embryo transfer, and cryopreservation planning
- Patient instructions, counselling notes, and follow-up scheduling
” The AI doesn’t diagnose. It doesn’t prescribe. It doesn’t make clinical decisions. It listens, understands, and documents, so you can focus entirely on the patient in front of you. “
The Doctor Is Always in Control
Every AI-generated note requires explicit physician review and approval before it enters the medical record. The final note carries the physician’s clinical authority because the physician approved it. This satisfies medical-legal requirements across the Middle East, Southeast Asia, Turkey, and other target markets, and is the principal reason physician adoption rates are consistently high.

The Problem It Solves And Why IVF Clinics Feel It Harder Than Most
Every physician knows documentation is heavy. But IVF physicians carry a load that is categorically different. A routine GP note is brief. A single IVF consultation requires stimulation protocol details, antral follicle counts, medication dosages and timing, previous cycle outcomes, semen analysis results, endometrial thickness, embryo development observations, transfer planning, and personalised follow-up, all in the correct structured EMR fields, all in real time.
The need to reduce documentation time in IVF is not a marginal efficiency goal; it is a clinical sustainability issue. The scale of that burden, compounded across 10 to 15 consultations a day, has consequences the data makes impossible to ignore.
Burnout Is the Hidden Business Risk With a Price Tag
Physician burnout documentation is no longer a well-being metric; it’s a financial and operational risk. A 2025 JAMA Network Open study led by Yale School of Medicine, tracking 263 physicians across six US healthcare systems, found that over half, 51.9%, were experiencing burnout before any intervention. Documentation burden was cited as the primary driver.
When a fertility specialist burns out, the cost of replacing them runs between USD 800,000 and USD 1.3 million. In a specialty already under global supply pressure, that is a business problem, not a wellness problem.
51.9% → 38.8% physician burnout rate, after just 30 days of AI scribe adoption across 6 healthcare systems.
Source: Olson et al., JAMA Network Open, October 2025
74% lower odds of experiencing burnout with AI scribe use, the largest burnout intervention result in physician wellness research.
Source: Olson et al., JAMA Network Open, October 2025
What the Patient Experiences, Even If They Never Say It
There is a dimension to this problem that doesn’t appear in any operational report, but IVF patients feel it acutely. When a doctor’s attention is split between the patient and the screen, trust erodes quietly. A large-scale Permanente Medical Group study published in NEJM Catalyst found that 84% of physicians using AI scribes reported a positive effect on patient communication, and nearly half of patients said their doctor spent less time looking at a computer. In IVF, where the consultation is the foundation of the patient relationship, that shift directly affects retention and outcomes.
Why Generic AI Scribes Fall Short and What IVF Clinic Documentation Software Must Do Differently

If you’re actively evaluating platforms, here is what separates a genuine AI scribe fertility clinic solution from a general-purpose tool with a new label: choosing the right AI medical scribe for IVF is not the same decision as choosing AI documentation software for general medicine. The majority of platforms were built for primary care and hospital medicine. In a fertility setting, that creates three structural gaps, each with real clinical and operational consequences.
Terminology: Why Medical Transcription Software for Fertility Clinics Must Be Specialty-Trained
General speech recognition and medical transcription software are trained on primary care and hospital language. It frequently mishandles fertility vocabulary, antral follicle count, blastocyst grading, luteal phase support protocols, ICSI, controlled ovarian hyperstimulation, and endometrial receptivity assays. A scribe who mishears clinical terminology doesn’t save time. It creates a correction burden your team must absorb. You haven’t eliminated the documentation burden; you’ve relocated it.
Integration: Where IVF Clinic Documentation Software Must Deliver
Many platforms produce a clean note in a separate application, requiring manual transfer into your EMR. That is half a solution. For the full value to land, IVF clinic documentation software must populate structured fields directly in the EMR your team already uses. Not a text dump. Not a PDF. Stimulation protocol data into the protocol section. Embryology observations into the lab record. Automatically.
Consistency: The Quiet Crisis for Multi-Location Fertility Clinics
When consultants document differently, patient records become incomparable across physicians and locations, a direct risk to clinical quality, coordinated care, and regulatory compliance. An AI scribe embedded in a shared IVF EMR enforces structural consistency across every consultation in every fertility clinic in your network. Every physician, every location: identically structured records, every time.
| Dimension | ❌ Generic AI Scribe | ✅ IVF-Native AI Scribe |
| Speech recognition | General medicine only | Trained on IVF/ART terminology |
| EMR output | Separate app — manual transfer | Native fields auto-populated |
| Note structure | Generic SOAP format | IVF-specific clinical sections |
| Team consistency | Varies by physician | Identical across all consultants |
| Lab data linkage | Fragmented, hard to correlate | Clean linkage to embryology records |
| Data usability | Limited analytics value | Clean, outcomes-ready data |
| After-hours charting | Partially reduced | Near-eliminated |
What This Means for the Embryology Lab, Not Just the Consultation Room
Most coverage of AI medical scribes for IVF stops at the consultation room. That misses half the picture, especially for embryologists and lab directors who work directly downstream from clinical documentation.
When a consultant’s notes are inconsistent, abbreviated, or missing key details, stimulation response, endometrial thickness, oocyte maturity, sperm parameters, the embryology team works with incomplete information. Decisions about fertilisation strategy, embryo culture conditions, and transfer timing are made in a data environment shaped by how the consultant happened to document that day.
When every consultation produces the same structured, complete record, with the same fields populated in the same format, the embryology lab receives reliable, comparable upstream data. This means:
- Cycle-to-cycle correlations become meaningful because the clinical data is structured consistently
- Embryologist access to prior cycle notes is faster and more complete, no more deciphering abbreviated free text
- Lab outcome data can be correlated cleanly against clinical variables, building a real foundation for outcomes analytics
- Multi-physician clinics stop having documentation quality vary by consultant; the lab sees the same record regardless of who ran the consultation
🔬 A Note for Lab Directors and Embryologists
Clean upstream documentation is a data quality issue, not just a clinical workflow issue. The structured notes an AI medical scribe for IVF generates are the same notes your outcomes analytics depend on.
For any clinic serious about building an evidence base for its protocols, AI documentation isn’t optional infrastructure; it’s the foundation.
The Real-World Impact: What the Evidence Actually Shows
The evidence base has crossed the threshold from ‘promising’ to ‘definitive.’ These are peer-reviewed findings from institutions whose research standards are not in question.
Physicians Get Their Evenings Back: How AI Scribes Reduce Charting Time
The Permanente Medical Group deployed AI scribes across 2.5 million patient encounters in 2023–2024. The result, published in NEJM Catalyst: nearly 15,800 physician hours saved in a single year, significant reduction in after-hours documentation, and improved patient–physician interaction quality, Kaiser’s fastest-ever technology rollout.
At Mass General Brigham, burnout prevalence fell by 21.2 percentage points at 84 days. More than one in five burned-out physicians recovered to non-burnout status from a single operational change. And critically, ambient AI clinical documentation was the mechanism behind every one of those gains.
” Our physicians tell us that they have their nights and weekends back and have rediscovered their joy of practicing medicine. There is literally no other intervention in our field that impacts burnout to this extent. “
— Rebecca Mishuris, MD — Chief Medical Information Officer, Mass General Brigham (JAMA Network Open, 2025)
Cleaner Data. Sharper Analytics. Better Clinical Outcomes.
Structured AI-generated notes transform the EMR from a documentation repository into an outcomes intelligence platform. Clinical note automation, the process of converting spoken consultations into structured, field-level records without manual input, means every consultation produces consistently formatted data across every consultant, every site, every cycle. IVF success rates by stimulation protocol. Medication response patterns by patient cohort. Embryo quality correlations. These have always been theoretically possible. AI documentation makes them operationally real.

The Three Concerns Every Clinic Leader Raises, Answered
‘Is patient data safe?’
Reputable platforms operate under healthcare-grade compliance, HIPAA, and equivalent regional standards. Audio is not stored post-consultation. Data is encrypted in transit and at rest. For fertility clinics in the UAE, Saudi Arabia, Malaysia, and Turkey, confirm that the platform supports local data residency requirements. This is standard in enterprise-grade solutions.
A useful reframe: the informal documentation practices an AI medical scribe for IVF replaces, notes on personal devices, handwritten shorthand, shared screens, often carry higher data risk than a purpose-built, compliant platform.
‘Will our doctors actually use it?’
Adoption data is consistent across all major deployments. At Mass General Brigham, 95% of providers who offered ambient AI clinical documentation took it up. A 2025 JAMIA survey of 43 US healthcare systems found it was the only AI use case with 100% adoption. Most physicians report the ability to reduce charting time within their first week and feel natural with the review-and-approve workflow almost immediately.
‘Is this mature enough for a specialty as complex as IVF?’
It depends entirely on the platform. Generic scribes carry documented failure modes in a fertility setting: terminology errors, incomplete data extraction, and poor EMR field alignment. A dedicated AI scribe fertility clinic solution, built natively inside an IVF EMR, trained on reproductive medicine language, mapped to IVF-specific clinical fields, is a different proposition entirely. The question to ask any vendor: Was this built for IVF, or adapted to it?
What to Ask Before You Choose an AI Medical Scribe for Your Fertility Clinic
Not every AI medical scribe for IVF will deliver what it promises. Whether you’re comparing an AI scribe fertility clinic platform against a generic solution, or evaluating a first-time deployment, these five questions cut straight to implementation reality:
- Is speech recognition trained specifically on IVF and reproductive medicine, or is it a general medical model?
- Does the scribe integrate natively into your EMR, auto-populating IVF-specific structured fields, or does it produce a document that still needs manual transfer?
- What does physician review actually take per consultation, and what is the error correction process?
- How does the platform handle healthcare data privacy compliance in your jurisdiction?
- Can it maintain a consistent documentation structure across multiple consultants and clinic locations?
🩺 About MedAI Scribe by Meddilink
MedAI Scribe is Meddilink’s AI medical scribe for IVF clinics, built natively inside the MedART EMR, the clinical management platform designed specifically for IVF and ART practices. It supports the complete fertility clinic workflow automation lifecycle: from voice-to-EMR transcription during consultation to structured embryology records and outcomes reporting, all without a single manual step.
Currently available for MedART EMR users. For clinics not yet on MedART, our team can walk you through what a transition looks like, starting with the documentation layer.
A Global Shift Already Underway and a First-Mover Window That Won’t Stay Open
Global AI in healthcare investment is forecast to grow from USD 21.66 billion in 2025 to USD 110.61 billion by 2030, a 38.6% CAGR. Ambient AI clinical documentation is the single largest category of that investment at an estimated USD 600 million annually, accelerating into specialty medicine at a pace. The IVF market is expanding sharply, valued at USD 32 billion in 2025, forecast to reach USD 68.57 billion by 2034 (Precedence Research).
The Middle East, Southeast Asia, Turkey, The Opportunity No One Has Claimed Yet
The UAE and Saudi Arabia’s Vision 2030 programmes have identified AI-assisted clinical documentation as a national healthcare priority. Thailand, the region’s leading IVF tourism hub, makes patient experience a direct competitive differentiator. Turkey’s international patient base demands documentation consistency that meets global accreditation standards. In Russia and Kazakhstan, the English-language clinical technology conversation is almost entirely uncontested.
And across all of these markets, the AI medical scribe for the IVF space remains virtually unclaimed. No AI scribe fertility clinic platform from the US or European market has established a meaningful presence in fertility clinics across the Middle East and Southeast Asia. Fertility medicine is running 12 to 18 months behind general medicine on AI documentation adoption. The clinics that move now will have three years of clean, structured outcomes data before their competitors have even started a pilot.
The Bottom Line For Every Decision-Maker in the Room
The evidence is settled. Studies from Yale, JAMA, Mass General Brigham, NEJM Catalyst, and UCLA converge on the same conclusion: ambient AI documentation reduces burnout, reclaims clinical hours, improves patient experience, and generates cleaner data without removing physician oversight.
But the case looks different depending on where you sit:
🩺 For Physicians and Fertility Specialists
An AI medical scribe for IVF gives you back the one thing no salary increase or scheduling change has managed to return: your full attention in the consultation room. The appointment becomes a conversation again, not a documentation exercise.
🔬 For Embryologists and Lab Directors
Clean, consistent upstream documentation means your lab data finally has a reliable clinical record to correlate against. Every stimulation detail, every cycle variable structured, comparable, and accessible. That’s your outcomes analytics infrastructure.
💼 For CEOs, CTOs, and CXOs
This is a revenue capacity, retention, and competitive differentiation decision. More consultations per day. Avoided physician replacement costs. Cleaner data for accreditation. A first-mover advantage in a specialty where your region’s AI scribe space is almost entirely unoccupied. The window is open, but it will not stay open indefinitely.
An AI medical scribe for IVF doesn’t change what a great fertility specialist does. It changes how much of that specialist’s time is consumed by a keyboard. In a specialty where the quality of the consultation is the most powerful variable in the room, that is not a marginal operational improvement. It is a strategic one.





