Over the past decade, fertility clinics across Central Asia have experienced steady growth. Rising awareness of reproductive health, expanding urban healthcare infrastructure, and increasing access to assisted reproductive technologies have contributed to higher patient volumes. Yet, while clinical demand has evolved, many operational systems have remained largely unchanged.
This case study examines the challenges of legacy EMR in fertility clinics and how one multi-location IVF clinic in Kazakhstan addressed them through structured digital transformation. Rather than focusing on technology alone, the transformation centred on workflow efficiency, clinical collaboration, patient engagement, and long-term scalability.
For IVF clinic decision makers, this account offers practical insight into how digital infrastructure can support both clinical excellence and organisational growth.
Organisational Context
The clinic operated several fertility centres across major cities in Kazakhstan. Its services included diagnostic fertility assessments, IVF and ICSI cycles, embryo transfer, cryopreservation, and related reproductive treatments. Over time, the organisation expanded rapidly to meet growing patient demand.
While clinical expertise remained strong, operational systems struggled to keep pace. Each branch relied on locally installed desktop software for patient records and administrative tasks. These systems were not connected across locations and were not designed specifically for IVF workflows.
As patient volumes increased, three systemic challenges became increasingly visible:
- Information fragmentation across locations
- Manual, time-consuming clinical workflows
- Limited digital engagement for patients
Leadership recognised that sustaining growth without improving digital infrastructure would eventually compromise both efficiency and quality of care.
Fragmented Clinical Data: One of the Core Challenges of Legacy EMR in Fertility Clinics
Each clinic branch maintained its own patient records. When patients moved between locations—or when doctors collaborated across cities—complete medical histories were not always accessible.
This fragmentation created both clinical and operational risks. Doctors often had to rely on partial information, slowing decision-making and reducing continuity of care. Administrative teams spent significant time requesting records from other branches, duplicating documentation, and reconciling inconsistencies.
From a governance perspective, leadership lacked a unified view of patient journeys, treatment outcomes, and operational performance across the network.
By centralising patient records within MedART, the clinic established a single source of truth. Authorised clinicians could access the same up-to-date information regardless of location, improving collaboration, clinical confidence, and organisational oversight.
Manual Laboratory Integration
Laboratory data plays a critical role in IVF treatment. Hormone levels, embryology reports, and diagnostic results directly influence clinical decisions. Yet, the clinic’s previous workflows relied heavily on manual uploads and disconnected systems.
Lab technicians often had to export results and share them through separate platforms or physical documents. This introduced delays, increased administrative workload, and created opportunities for transcription errors.
Clinicians, in turn, had to wait for reports to be uploaded before adjusting treatment plans. In time-sensitive IVF cycles, even minor delays can affect outcomes and patient confidence.
Integrating laboratory systems with MedART allowed results to flow automatically into patient records. This reduced turnaround time, improved data accuracy, and ensured that doctors could act on real-time information.
For IVF clinic decision makers, this integration strengthened both clinical precision and operational efficiency.
Paper-Based Consent and Documentation
Consent management is a critical aspect of reproductive care, involving multiple forms for procedures, storage, and treatment approvals. Previously, these documents were handled through physical files and manual processes.
This approach created several challenges:
- Delayed patient onboarding
- Difficulty retrieving documents
- Increased risk of misplaced records
- Limited audit visibility
Staff spent unnecessary time searching for files, while patients experienced longer administrative processes.
Digitising consent forms through MedART created a structured, secure, and easily accessible system. Documents could be uploaded, signed, and stored within the patient’s digital record, improving compliance and efficiency.
This shift reduced paperwork, strengthened data security, and improved the overall patient experience.
Limited Patient Access to Information
Patients previously depended on phone calls or in-person visits to receive updates about their treatment. This created friction for both patients and staff.
Administrative teams handled a high volume of routine queries, such as appointment confirmations, report requests, and prescription details. Patients, meanwhile, often experienced delays in accessing their own health information.
The introduction of the patient app transformed this dynamic. Patients gained secure, real-time access to their reports, appointments, and treatment history. They could also communicate directly with care coordinators through a digital channel.
This improved transparency, reduced communication bottlenecks, and strengthened patient trust.
Leadership Visibility Gaps
For IVF clinic decision makers, operational visibility is essential for strategic planning. Without a centralised system, leadership lacked access to consistent, real-time data across all branches.
Key questions were difficult to answer:
- How are different locations performing?
- Where are workflow bottlenecks occurring?
- How efficiently are resources being used?
- What trends are emerging in patient engagement?
MedART provided leadership with a unified view of operations. With consistent data across branches, decision makers could make informed choices about staffing, expansion, and process improvements.
This shift moved leadership from reactive management to proactive planning.
Defining Transformation Objectives
Rather than pursuing a generic “digital upgrade,” the clinic focused on clearly defined operational goals:
- Centralise patient data across all locations
- Digitise IVF-specific clinical workflows
- Integrate laboratory systems with the EMR
- Improve patient communication and transparency
- Build a scalable digital foundation
These objectives emphasised process improvement over technology adoption alone.
Download the Full Kazakhstan Case Study
For a deeper, data-supported view of this transformation, IVF clinic decision makers can download the complete Kazakhstan case study.
The full report provides:
- Implementation timelines
- Workflow comparisons
- Operational insights
- Transformation outcomes
This allows clinic leaders to explore how structured digital transformation can support long-term growth in fertility care.
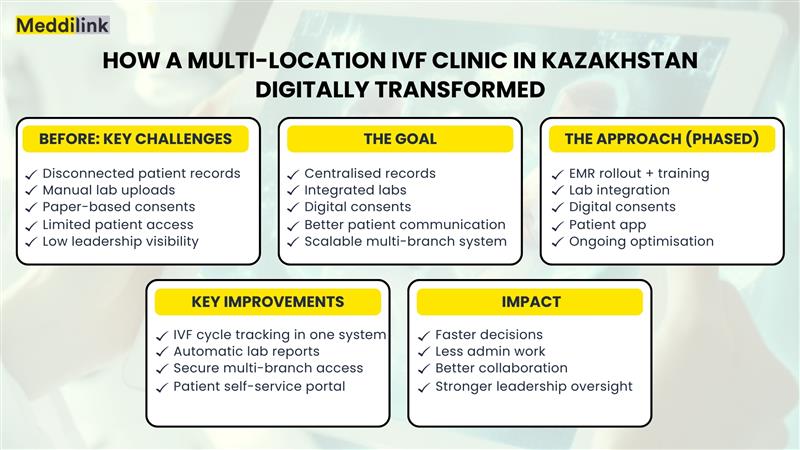
Implementation Strategy: A Phased, Human-Centred Approach
The transformation followed a phased model designed to minimise disruption and support staff adoption.
Phase 1: Centralising Clinical Records
The first step was to unify patient data across all branches.
MedART enabled:
- Shared access to patient histories
- Digital clinical notes
- IVF cycle tracking
- Secure multi-location data visibility
Doctors working in different cities could now view consistent, up-to-date patient information. This improved clinical coordination and reduced duplicated documentation.
Training focused on helping staff understand how digital workflows could simplify, rather than complicate, their daily tasks.
Phase 2: Integrating Laboratory Systems
In-house laboratory systems were connected directly to MedART.
This allowed:
- Automatic upload of test results
- Real-time data availability
- Reduced manual entry
Embryologists and clinicians gained faster access to diagnostic information, enabling more timely treatment decisions. Operationally, this reduced administrative overhead and improved data accuracy.
Phase 3: Digitising Consent and Documentation
Consent forms and treatment documents were moved into a secure digital format.
Benefits included:
- Faster patient onboarding
- Easier document retrieval
- Improved compliance tracking
Patients experienced smoother administrative processes, while staff spent less time managing physical files.
Phase 4: Introducing the Patient App
The patient app improved communication and transparency.
Patients could:
- View lab reports
- Check appointments
- Access prescriptions
- Review treatment history
- Communicate securely with coordinators
This reduced call volumes and allowed staff to focus on clinical support rather than administrative queries.
Phase 5: Ongoing Optimisation
Post-implementation, the clinic continued refining workflows based on staff feedback and operational needs.
System updates focused on:
- Workflow efficiency
- Data usability
- Reporting clarity
- User experience improvements
Transformation was treated as a continuous process, not a one-time event.
Clinical Workflow Improvements
IVF Cycle Tracking
Doctors gained structured visibility into each patient’s treatment journey. Protocols, stimulation schedules, and progress notes were documented within a single system.
This improved:
- Clinical clarity
- Treatment consistency
- Cross-team communication
Multi-Branch Collaboration
With shared access to patient data, doctors across locations could collaborate more effectively. Case discussions, second opinions, and continuity of care improved significantly.
Patient Engagement
Digital access to personal health information increased patient confidence and transparency. Patients felt more informed and involved in their treatment process.
Impact on Leadership Decision-Making
For IVF clinic decision makers, the most significant change was operational visibility.
Leadership gained access to:
- Unified data across branches
- Workflow performance insights
- Patient engagement patterns
- Resource utilisation trends
This supported:
- Better strategic planning
- Improved quality control
- Informed expansion decisions
Rather than reacting to operational challenges, leadership could proactively address them.
Outcomes
The transformation was measured in operational improvements rather than marketing metrics:
- Faster access to lab results
- Reduced administrative workload
- Improved staff coordination
- Better patient communication
- Stronger data governance
The clinic did not merely adopt technology.
It redesigned how care was delivered.
Conclusion
For many growing organisations, the challenges of legacy EMR in fertility clinics are not technical alone, they are operational, clinical, and strategic.
This case from Kazakhstan demonstrates that meaningful transformation is not driven by software alone. It requires:
- Clear operational goals
- IVF-specific workflows
- Phased implementation
- Continuous staff engagement
- Leadership commitment
MedART supported the clinic’s clinical expertise rather than replacing it. The result was a system that strengthened both operational performance and patient care.
For IVF clinic decision makers, the lesson is clear:
Digital infrastructure must evolve at the same pace as clinical growth.





